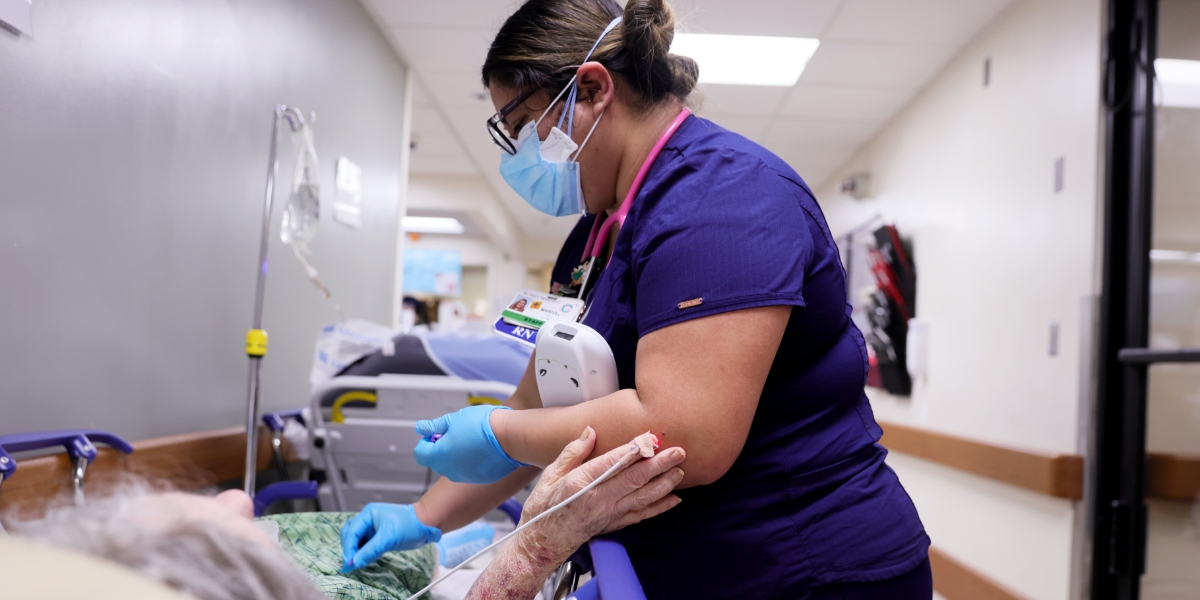
Following a successful COVID-19 vaccine rollout, occupancy levels at long-term care facilities are starting to inch upwards, with recent data showing the national median occupancy for skilled nursing facilities (SNFs) at 69.7% as of the end of February, compared with 69.2% at the end of January.
But even as occupancy levels start to rise again, providers at long-term and post-acute care (LTPAC) facilities continue to grapple with the economic fallout and other lingering side effects of the pandemic. While the clinical pandemic is fortunately coming to an end for some, the financial impacts remain for all.
For this reason, it’s critical that SNFs master the patient transition from the hospital. Providers must have a deep understanding of care needs, quantify the financial impact prior to patient arrival, and create efficiencies at every step in the process. By optimizing the admission process, facilities can ensure that every transfer is timely, accurate, and safe.
Three Steps for a Successful Transition
The economic impact of the pandemic means that long-term care facilities have to be more nimble to ensure that their organization remains successful and financially healthy.
With this in mind, there are three key things care facilities must do to optimize patient transitions from hospital to SNF:
1. Gain full visibility into your patients:
The first steps are to review the patients coming from the hospital to determine if the facility is able to treat them clinically and to validate their pre-admission information.
To do this efficiently, caregivers must have quick access to data and simple workflows that allow easy action and smart decisions. Connecting to an interoperability framework gives providers full visibility and access to a patient’s complete medical history. This includes COVID-19 vaccinations, lab results, and diagnosis information of referrals and incoming residents along with their clinical information, documents, and medications.
2. Mitigate financial liability and maintain a healthy referral pipeline:
It’s critical that facilities verify insurance coverage and communicate financial obligations before the patient is discharged from the hospital. Failure to do this in advance could leave nurses at risk of not being reimbursed for the care delivered or leave the facility at risk for out-of-pocket expenses.
According to the Healthcare Billing and Management Association, the estimated cost of managing denials is $25 per claim. Care providers must protect their revenue flow from coverage denials with an integrated insurance validation service that checks and monitors insurance coverage of current and potential residents to verify financial status.
3. Get it right in the first 48 hours
The change in care setting from acute to post-acute is one of the most vulnerable times in the patient journey. Therefore, it’s essential that they, along with their family or caregiver, know the facility is focused on healing and quality of life.
To start off on the right foot, ensure that a staff member greets the patient upon arrival and helps them to get settled in their room. Once confirming the assigned nurse has consent to treat the patient, the nurse should sign the necessary paperwork, capture immediate orders for the pharmacy, establish infection prevention and drug resistance protocols if needed, and perform a medical assessment. These are all crucial steps to fully understanding the new resident’s health picture from day one and providing the best possible care.
Having an effective care transition process helps facilities thoroughly identify patient needs, desired outcomes and payer sources. Getting it right from the start results in shorter stays, no emergency visits, no readmissions, no penalties, and no damage to reputation.
Prove Capabilities to Establish Strong Partnerships
In the wake of the economic fallout of the pandemic, it will be more important than ever for SNFs to take the lead in their relationships with hospitals. They will need to market their capabilities effectively to prove themselves as a strong partner. By promoting a high quality of care and better outcomes, long-term care facilities will maintain a healthy referral pipeline and bounce back more quickly.