Build a holistic view of your organizational performance. Advanced Insights offers organizational visibility of clinical, financial and operational metrics to drive reimbursement, enhance resident care, and improve quality.

Drive Efficiency Across Your Organization
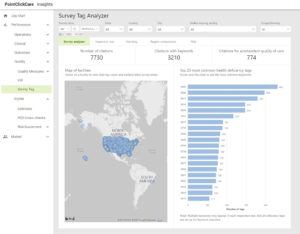
Interactive reports offer a comprehensive view into overall business performance both internally and within your market to address areas of performance improvement and enhance quality outcomes.

Ensure Accurate Reimbursement
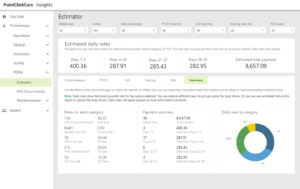
Leverage precise clinical reimbursement information to attain financial success and secure reimbursement for exceptional care provided.

Optimize Operational Outcomes
Easily access comprehensive analytics that are updated daily with the latest clinical documentation and MDS assessments.

What is Advanced Insights?
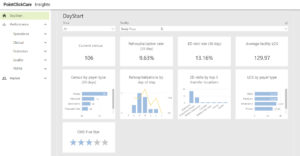
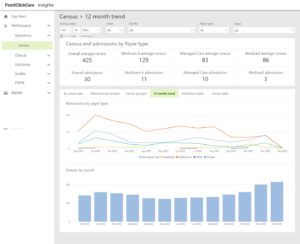
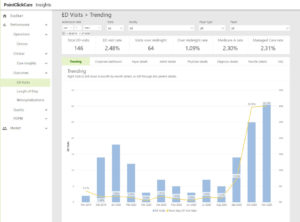
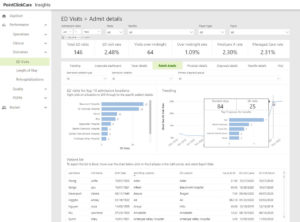
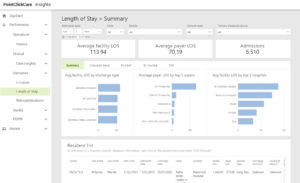
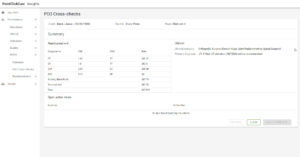
Advanced Insights offers data visualization embedded into your EHR platform, providing your organization with increased visibility of clinical, financial, and operational metrics. This innovative tool enhances patient care, improves quality, and drives reimbursement.
Interactive Operational Reports
Performance Insights help make complex data accessible and actionable at the corporate, facility and resident level. Learn more about the Predictive Return to Hospital (PRTH) risk report or additional reports to help with your operational reporting and monitoring.
Interested in learning more about Advanced Insights?
Request a Demo.