Additional Product
Eligibility Verification for Senior Living
Eligibility Verification is an integrated insurance validation service which helps organizations check and monitor supplemental payer coverage of current and prospective residents to verify financial status both prior to and post move-in.
Protect Your Revenue with Real-Time Coverage Insights
Improve Efficiency
Check multiple residents and insurance providers at once with real-time eligibility verification.
Minimize Non-Payment
Automatically detect coverage changes with weekly batch checks, eliminating reliance on families to report cancellations or policy updates.
Monitor Resident Mix
Gain visibility into your resident population with historical coverage reports that help you understand your resident mix.
Streamline Workflows
Access resident insurance data directly within your EHR platform, eliminating manual data entry and reducing errors.
Integrated Insurance Verification
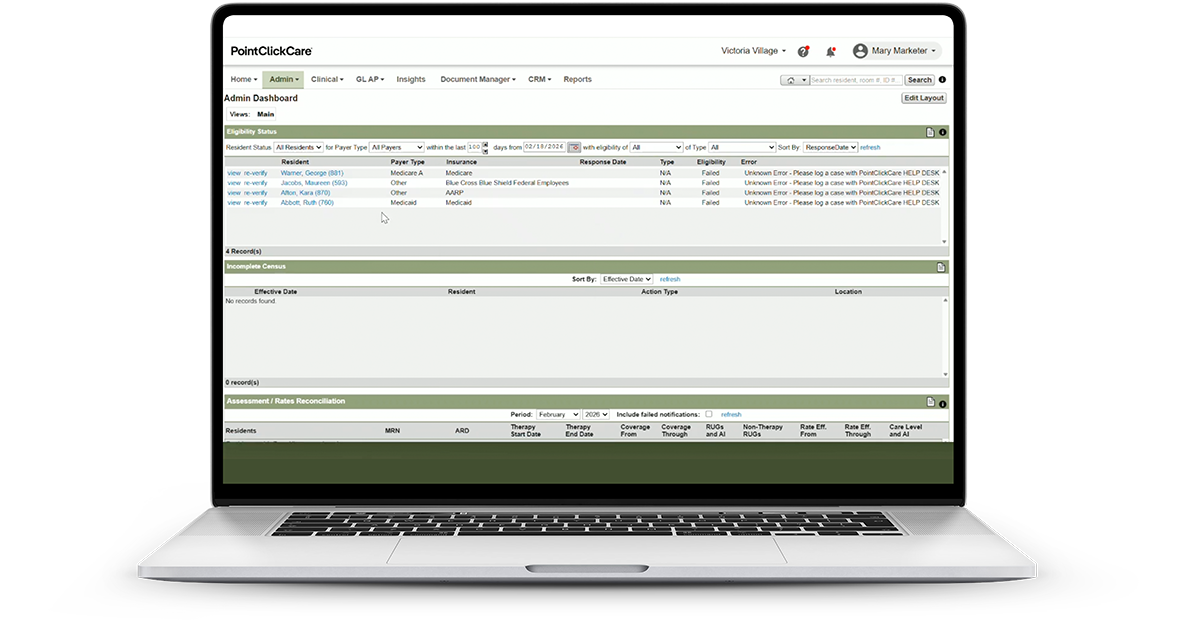
Verify Coverage in Real-Time Before and After Move-In
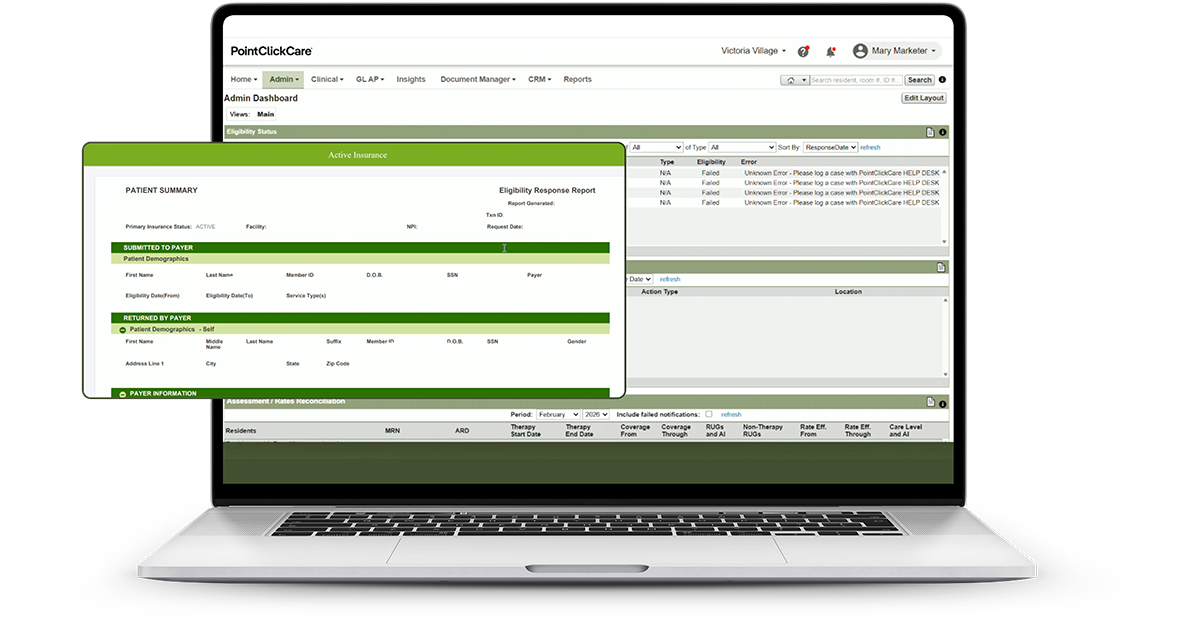
Instant Access to Insurance Data
Obtain real-time access to resident insurance eligibility through a solution that integrates directly with your PointClickCare EHR.
Automate Weekly Coverage Checks Across Your Entire Census
Automatic Batch Processing
Schedule automatic weekly batch reports that verify insurance coverage for all residents, saving you hours of administrative time.
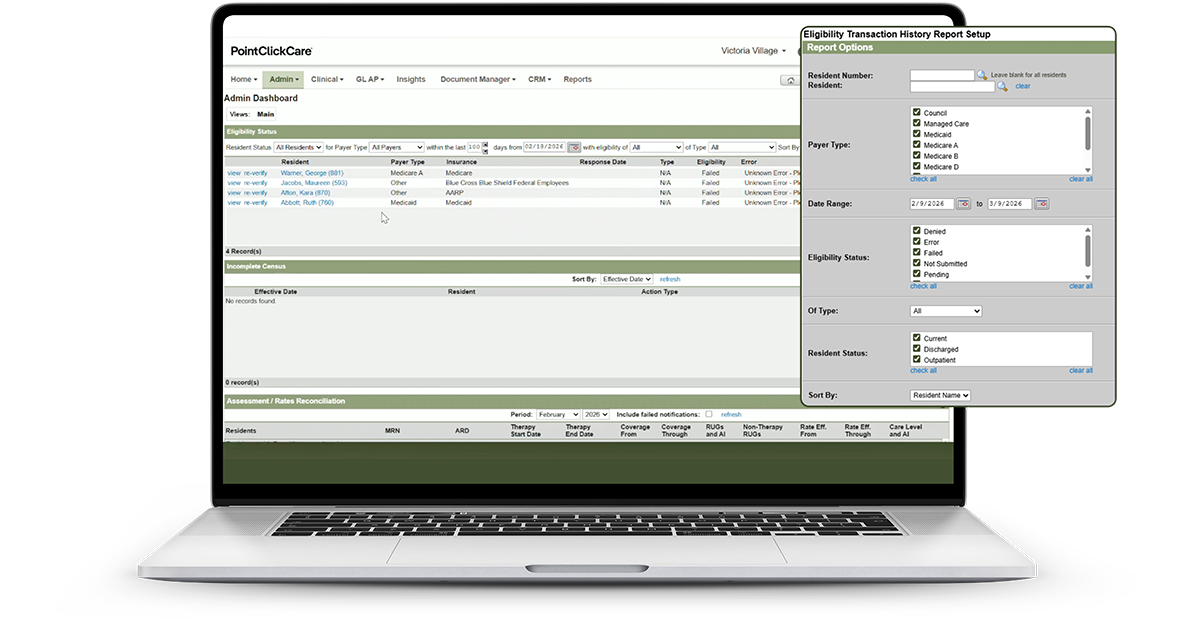
Understand Your Resident Mix with Metrics and Trends
Historical Coverage Reporting
Access current and historical insurance reports that provide clear visibility into coverage trends and resident demographics.
Verify Coverage in Real-Time Before and After Move-In
Instant Access to Insurance Data
Obtain real-time access to resident insurance eligibility through a solution that integrates directly with your PointClickCare EHR.

Automate Weekly Coverage Checks Across Your Entire Census
Automatic Batch Processing
Schedule automatic weekly batch reports that verify insurance coverage for all residents, saving you hours of administrative time.

Understand Your Resident Mix with Metrics and Trends
Historical Coverage Reporting
Access current and historical insurance reports that provide clear visibility into coverage trends and resident demographics.

Request a Demo
Request a demo to see how Eligibility Verification can help your organization minimize payment risk and optimize revenue cycle management.
Additional Product
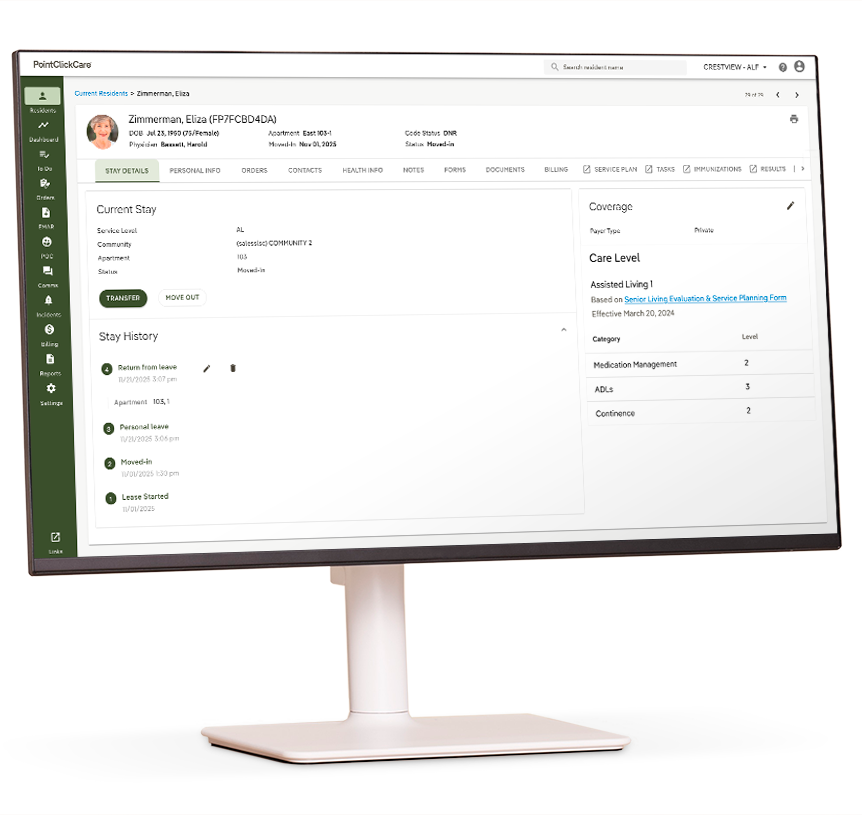
Eligibility Verification Expands the Capabilities of Your EHR
PointClickCare Eligibility Verification integrates seamlessly with your existing EHR platform, delivering insurance coverage data directly within your daily workflow. Combined with your PointClickCare EHR and Billing solutions, it creates a unified revenue cycle management system.
Additional Products to Expand Your
EHR Capabilities
See All Relevant Solutions
Value Packages
Additional Products
Frequently Asked Questions
Eligibility verification software automates the process of checking insurance coverage status for residents in senior living communities. It electronically confirms active coverage, benefits, and policy details in real-time, reducing manual phone calls and administrative burden.
Automated eligibility verification electronically checks insurance coverage when new information is entered into your system or through scheduled weekly batch reports. The software retrieves current coverage information and alerts your team to any changes or issues requiring attention.
Real-time eligibility verification minimizes payment delays by automatically running weekly checks on supplemental payer coverage. It reduces administrative burden by checking multiple residents simultaneously.
Yes, PointClickCare Eligibility Verification integrates seamlessly with your PointClickCare EHR platform, providing instant access to insurance data within your existing workflow. No separate login or system switching required—coverage information appears directly where you need it.
By verifying coverage for supplemental payers before move-in and throughout a resident’s stay, eligibility verification software helps you identify coverage issues before they result in denied claims. You can proactively address policy cancellations, coverage changes, and eligibility gaps.
Take a Closer Look
Request a demo of Eligibility Verification and see the difference streamlining admissions can make for your organization.